Assessing diastolic function in small animals is relatively simple to do and has powerful diagnostic and prognostic implications. It has been shown to predict congestive heart failure in dogs with myxomatous mitral valve disease (Kim & Park, 2015) and dilated cardiomyopathy (O’Sullivan et al., 2007), and be highly correlated with aortic stenosis severity in boxers even in the presence of normal systolic function (Schober and Fuentes, 2002). It may also be predictive of conditions like hypertrophic cardiomyopathy before it becomes apparent on 2D echo, and diastolic dysfunction often precedes systolic dysfunction as assessed by conventional measures such as ejection fraction.
Despite all of this work, it is surprisingly underused in clinical practice. This is in part due to the limitations of some machines (the presence or quality of their tissue Doppler imaging, in particular), the lack of normal values for different breeds, but also due to the fact that it is not routinely taught and performed. As with everything in echocardiography, repetition is the only way to gain skill and confidence in a new technique. For this reason, it’s important to implement any new measurement into your scanning protocol even on patients when it seems unnecessary or superfluous, if sufficient reproducibility is to be achieved for it to have any real diagnostic utility. This is easier said than done on feline patients, but dogs are generally tolerant enough that adding an extra couple of minutes onto their standard examination time will not cause undue distress.
In the below article, the normal mitral inflow pattern is described, as well as the normal myocardial excursion as assessed by Tissue Doppler Imaging (TDI). There is a guest video tutorial from David Dawson, Echocardiographer at Imperial College, demonstrating the process for obtaining each of these measurements. If you would be interested in learning about any of the these measures in greater depth, please reply to your newsletter email or use the contact form at the footer of this page to get in touch. We welcome all feedback so that we can ensure that our newsletters are relevant and useful to you.
In the video below, David Dawson describes how to take the perfect mitral inflow trace, septal TDI, and lateral wall TDI.
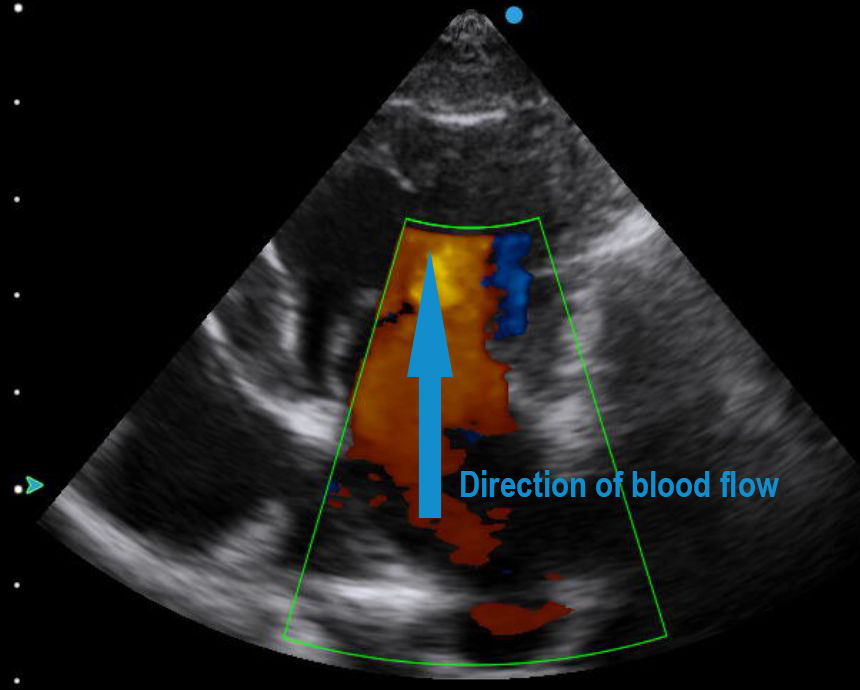
The mitral inflow trace is obtained from the left lateral decubitus position by placing the pulsed wave sample volume at the tips of the mitral valve, as demonstrated in the above video. Blood is flowing from the left atrium into the left ventricle towards the apex of the heart and therefore the transducer, so the baseline of the spectral Doppler trace is shifted downwards to allow the forward flow to occupy this space.
Three key measurements can be taken from this trace: E wave velocity, E wave deceleration time, and A wave velocity. Each of these measures have multiple uses across a variety of conditions – E wave velocity, for example, can be used as a supporting measurement for grading the severity of mitral regurgitation – but today’s focus will be on assessment of diastolic function.
Mitral inflow pattern
The E wave is the early filling component, and in the normal heart, this should reflect the suction of the left ventricle as it relaxes. The A wave is the late filling, or active component, occurring just after atrial contraction (the P wave on your ECG). In healthy dogs and cats, the E wave should always be higher than the A wave, meaning that the E/A ratio should always be greater than 1. Just as in older humans, in dogs over ten years of age the E/A ratio decreases (Boon, 2011), so an E/A ratio of around 1 in an older dog is not cause for alarm.
When you will not be able to calculate an E/A ratio: At very fast heart rates, there will be fusion of E and A waves, making the E/A ratio less useful in feline patients in particular. If you cannot calculate an E/A ratio on a cat, remember that you can be confident that there is some degree of diastolic dysfunction when there is a dilated left atrium and/or left ventricular hypertrophy. Isovolumic relaxation time (IVRT) is not altered by heart rate, so is one measure which can be consistently used in cats. IVRT can also be assessed by pulsed or continuous wave Doppler of the mitral inflow and aortic outflows, by bringing the baseline to the centre (to show flow both towards and away from the transducer) and moving your sample line or sample volume between the mitral inflow and aortic outflows so that you catch both in a single trace. IVRT is then measured from the closure click of the aortic valve, to the beginning of the mitral E wave. Delayed relaxation will lengthen IVRT, but once left atrial pressures become significantly elevated, IVRT will be shortened. The normal IVRT in canines is 41-73ms (de Madron, 2015).
If the animal is in atrial fibrillation, there will not be an A wave at all, so it will also not be possible to calculate an E/A ratio.

Normal values
Schober and Fuentes (2002) published normal values for Boxers as:
E/A ratio: 1.47 (0.95 – 2.22)
Deceleration time: 77ms (60-107)
E velocity: 0.76 m/s (0.53-0.96)
A velocity: 0.52 m/s (0.34 – 0.75)
BSA and body weight do not affect the transmitral inflow pattern (Boon, 2011), so its utility is not hindered by a lack of published data on one particular breed.
You should always be suspicious of a normal E/A ratio in an animal that you suspect has significant cardiac disease (e.g. in the presence of significant left ventricular hypertrophy), and check the deceleration time and TDI (discussed below). In more advanced diastolic dysfunction, the mitral inflow pattern may change from a reversed (A taller than E) to a ‘pseudonormal’ pattern, with a tall and steep E wave, and a diminutive A wave. The E wave returns to having a high velocity no longer due to the powerful suction forces of left ventricular relaxation (which is now stiffened and weak) but due to the elevated left atrial pressures creating a high pressure gradient between the left atrium and left ventricle.
In a pseudonormal pattern, E deceleration time will be short, E’ values (discussed below) will be very low, and E/E’ will therefore be high.
TDI measures the excursion of the myocardium, rather than the blood flow. TDI is less load dependent than the transmitral flow pattern. If your machine does not have a TDI setting, it is possible to create your own by adjusting your wall filters and PRF – just get in touch if you need help with this.
The TDI trace will show a systolic movement of the myocardium towards the transducer (“S prime”, denoted S’), and then E and A waves away from the transducer – hence below the baseline – referred to as “E prime” and “A prime”, denoted E’ and A’ (sometimes e’ and a’), respectively. The baseline in this instance is best positioned in the middle of your Doppler scale in order to show both the S’ component and the E’ and A’.

There is debate as to whether one should measure the septal E’ (sometimes referred to as sMVe’), the lateral E’ (pMVe’), or average the two. Even if you decide in your practice to use only one, it is useful – and will add only a few seconds onto your normal examination time – to routinely obtain both, as an insurance policy, if nothing else! There are cases, of course, where comparing the two can be extremely useful. Normally, septal E’ will be lower than lateral E’ because the septum has less freedom to move than the unrestrained lateral wall. In constrictive disease, however, the opposite will be the case because the lateral wall is tethered by the pericardium (this is termed annulus reversus).
With myocardial stiffening and delayed relaxation, E’ velocities reduce. Cats with HCM show a marked reduction in their E’ velocities (Koffas et al., 2006).
Hori et al. (2007) published normal values for the Beagle as:
Lateral E’: 7.4±1.8
Lateral A’: 3.3±1.2
Lateral E/E’ ratio 7.7±1.8
Septal E’: 5.5±1.1
Septal A’: 3.9±1.2
Septal E/E’ ratio 11.8±2.9
Calculating an E/E’ ratio is highly recommended as part of a minimum dataset of any echocardiographic examination.
As mentioned previously, your 2D imaging will often give you the first clues that diastolic function may not be normal, particularly in the presence of left atrial dilatation and left ventricular hypertrophy. Indeed, E/E’ ratios correlate with other key veterinary measures, such as LA/Ao in dogs with myxomatous mitral valve disease (Tidholm et al., 2009).
There are other Doppler measurements which will add to your diagnostic confidence, such as pulmonary venous flow pattern. If you’ve found this article useful and would like some further tutorials on assessing diastolic function, please sign up to our newsletter, arrange a free call, or consider our veterinary echocardiography training programme, which is packed full of demonstration videos in dogs and cats.
References
Boon, J., 2011. Veterinary Echocardiography, Second Edition. Blackwell Publishing, Ames, Iowa.
De Madron, E., 2015. Clinical Echocardiography of the Dog and Cat. Elsevier, St Louis, Missouri.
Hori, Y., Sato, S., Hoshi, F. et al., 2007. Assessment of longitudinal tissue Doppler imaging of the left ventricular septum and free wall as an indicator of left ventricular systolic function in dogs. Am J Vet Res (68):1051-1057.
Kim, J., Park, H., 2015. Usefulness of Conventional and Tissue Doppler Echocardiography to Predict Congestive Heart Failure in Dogs with Myxomatous Mitral Valve Disease. J Vet Intern Med, 29(1):132-140.
Koffas, H., Dukes-McEwan, B., Corcoran, C., et al. (2006). Pulsed Tissue Doppler Imaging in Normal Cats and Cats with Hypertrophic Cardiomyopathy. J Vet Intern Med (20):65-77.
O’Sullivan, M., O’Grady, M., Minors, S., 2007. Assessment of Diastolic Function by Doppler Echocardiography in Normal Doberman Pinschers and Doberman Pinschers with Dilated Cardiomyopathy. J Vet Intern Med (21):81–91.
Schober, K., Fuentes, V., 2002. Doppler echocardiographic assessment of left ventricular diastolic function in 74 boxer dogs with aortic stenosis. J Vet Cardiol., 4(1)7-16.
Tidholm, A., Ljungvall, I., Hoglund, A. et al. (2009). Tissue Doppler and Strain Imaging in Dogs with Myxomatous Mitral Valve Disease in Different Stages of Congestive Heart Failure. J Vet Intern Med (23):1197–1207.
© 2025 | AUA – All Rights Reserved
